Your message has been sent.
 CLOSE SIDEBAR
CLOSE SIDEBAR
Racial Disparities and Sociodemographic-Based Differences in Rhegmatogenous Retinal Detachment Presentation and Postoperative Outcomes
Pooja M. Shah
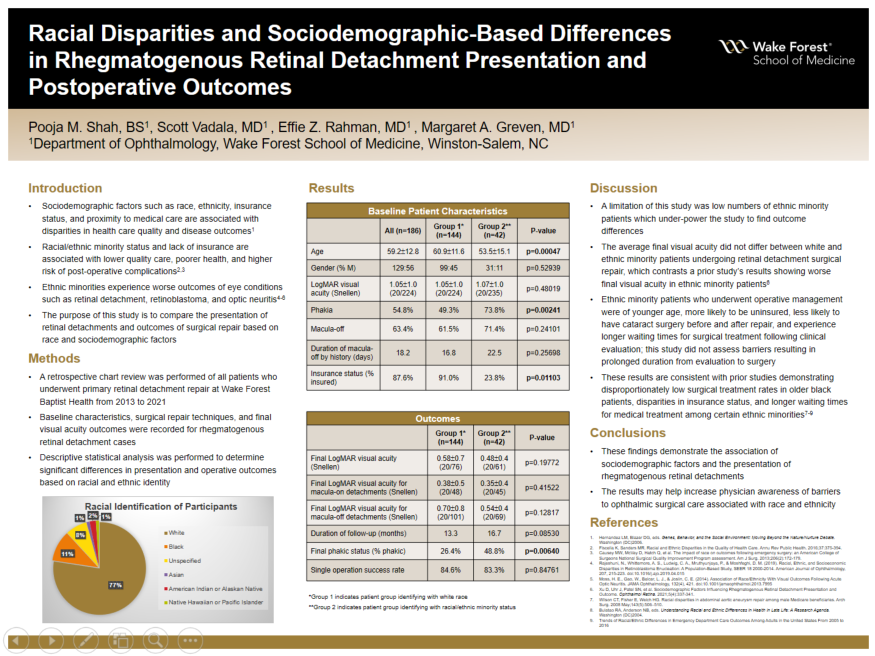
Background: Sociodemographic factors such as race, ethnicity, insurance status, and proximity to medical care are associated with disparities in health care quality and disease outcomes. Ethnic minorities experience worse outcomes of eye conditions such as retinal detachment, retinoblastoma, and optic neuritis. The purpose of this study is to compare the presentation of retinal detachments and outcomes of surgical repair based on race.
Hypothesis: Of all patients in our cohort undergoing retinal detachment surgery, racial and ethnic minorities will have poorer outcomes.
Methods: A retrospective chart review was performed of all patients who underwent primary retinal detachment repair at Wake Forest Baptist Health from 2013 to 2021. Baseline characteristics, surgical repair techniques, and final visual acuity outcomes were recorded.
Results: 186 eyes of 181 patients were included. 144 patients identified their race as white and 42 patients identified their race as Black, Asian, American Indian or Alaska Native, Native Hawaiian or Pacific Islander, Latin American or Hispanic, or unspecified non-white. Baseline characteristics including gender and baseline visual acuity were similar between the two groups. Age (p=.0005) and insurance status (p=.011) were statistically significant differences between the two groups. A greater proportion of white patients (15.8%) had operative treatment at ages 70-89 than non-white patients (9.5%). The average age difference between the two groups was 7.1 years. 91% of white patients had health insurance, while 23.8% of non-white patients had health insurance. The proportion of patients who presented with macula-off detachments did not differ by racial identity (p=.241). However, the time from evaluation to surgery was significantly longer in non-white patients (p=.027). Differences between the two groups in duration of visual acuity loss prior to presentation, visual outcomes in both macula-on and macula-off detachments, and total duration of follow up were not statistically significant. Average final visual acuity for all macula-on retinal detachments was logmar 0.375 (Snellen 20/47), logmar 0.38 (Snellen 20/48) for the group identifying as white, and logmar 0.35 (Snellen 20/45) for the group identifying as non-white. Average final visual acuity was logmar 0.6597 (Snellen 20/91) for all in macula-off retinal detachments, logmar 0.70 (Snellen 20/101) for the group identifying as white, and logmar 0.54 (Snellen 20/69) for the group identifying as non-white. Single operation success rate did not differ between the two groups.
Conclusions: Although the average final visual acuity did not differ between white and non-white patients undergoing retinal detachment surgical repair, non-white patients who underwent operative management were of younger age, more likely to be un-insured, less likely to have cataract surgery before and after repair, and experience longer waiting times for surgical treatment following clinical evaluation. These findings may help increase physician awareness and guide interventions to address barriers to ophthalmic surgical care associated with race.
Powered by Acadiate
© 2011-2024, Acadiate Inc. or its affiliates · Privacy
