Your message has been sent.
 CLOSE SIDEBAR
CLOSE SIDEBAR
Outcomes 2-Years After Hip Microfracture Augmented with Allograft Cartilage and Autologous Platelet Rich Plasma
Keon Youssefzadeh
Poster Title: Outcomes 2-Years After Hip Microfracture Augmented with Allograft Cartilage and Autologous Platelet Rich Plasma
Student: Keon Youssefzadeh, Class of 2024
Faculty Mentor and Department: Allston J. Stubbs IV, Department of Orthopaedic Surgery
Funding Source: Department of Orthopaedic Surgery, Wake Forest School of Medicine
ABSTRACT
Background: Articular cartilage injuries and early osteoarthritis of the hip joint, often as a result of femoroacetabular impingement (FAI), propose a unique challenge to surgeons. Due to its avascularity, articular cartilage exhibits a limited ability to regenerate itself. Acute damage or repeated insult of the cartilage may lead to progressive osteoarthritis (OA) of the hip joint, pain, and loss of function. For patients with these injuries, cartilage salvaging procedures and correction of bony morphology may provide a less invasive alterative to total hip arthroplasty (THA). In this study we examine the outcomes of acetabular microfracture augmented with allograft cartilage and autologous platelet rich plasma (PRP).
Hypothesis:Hip microfracture augmented with allograft cartilage and autologous platelet rich plasma will yield stable and significant improvement to hip outcome measures at a minimum 2-year time point.
Methods: Data from a prospective series of consecutive patients with Outerbridge grade IV chondromalacia of the acetabulum or femoral head who underwent acetabular microfracture augmented with allograft cartilage and autologous PRP from 2016 to 2019 was analyzed. Modified Harris Hip Score (mHHS), Hip Outcome Score Activities of Daily Living (HOS-ADL) HOS Sport-Subscale (HOS-Sport), Non-Arthritic Hip Score (NHS), visual analog scale (VAS) pain, and VAS satisfaction served as outcome measures for this study.
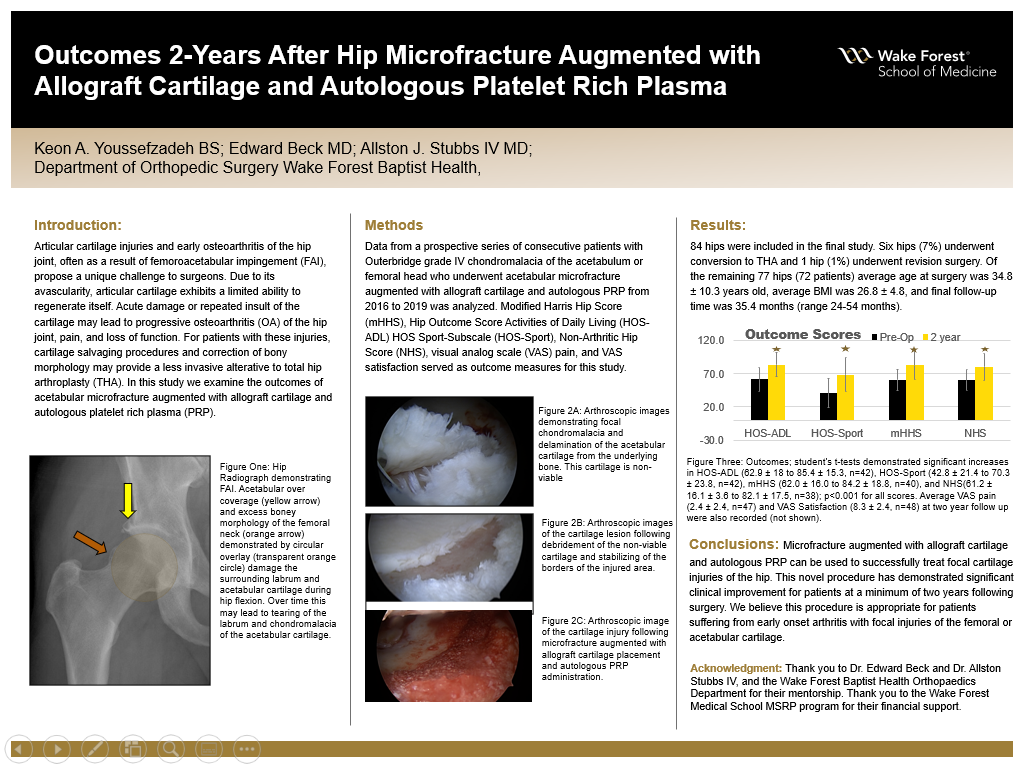
Results: 84 hips were included in the final study. Six hips (7%) underwent conversion to THA and 1 hip (1%) underwent revision surgery, and subsequently were excluded from further analysis. Of the remaining 77 hips (72 patients) average age at surgery was 34.8 ± 10.3 years old, average BMI was 26.8 ± 4.8, and final follow-up time was 35.4 months (range 24-54 months). Sixty-five (84%) had pre-operative scores available and 48 (62%) had minimum 2 year post operative sores available. Student’s t-tests demonstrated significant increases in HOS-ADL (62.9 ± 18 to 85.4 ± 15.3, n=42), HOS-Sport (42.8 ± 21.4 to 70.3 ± 23.8, n=42), mHHS (62.0 ± 16.0 to 84.2 ± 18.8, n=40), and NHS(61.2 ± 16.1 ± 3.6 to 82.1 ± 17.5, n=38); p<0.001 for all scores. Average VAS pain (2.4 ± 2.4, n=47) and VAS Satisfaction (8.3 ± 2.4, n=48) at two year follow up were also recorded.
Conclusions: Microfracture augmented with allograft cartilage and autologous PRP can be used to successfully treat focal cartilage injuries of the hip. This novel procedure has demonstrated significant clinical improvement for patients at a minimum of two years following surgery. We believe this procedure is appropriate for patients suffering from early onset arthritis with focal injuries of the femoral or acetabular cartilage.
Source of mentor’s funding or other support that funded this research: Department of Orthopaedic Surgery, Wake Forest School of Medicine.
Powered by Acadiate
© 2011-2024, Acadiate Inc. or its affiliates · Privacy
