Your message has been sent.
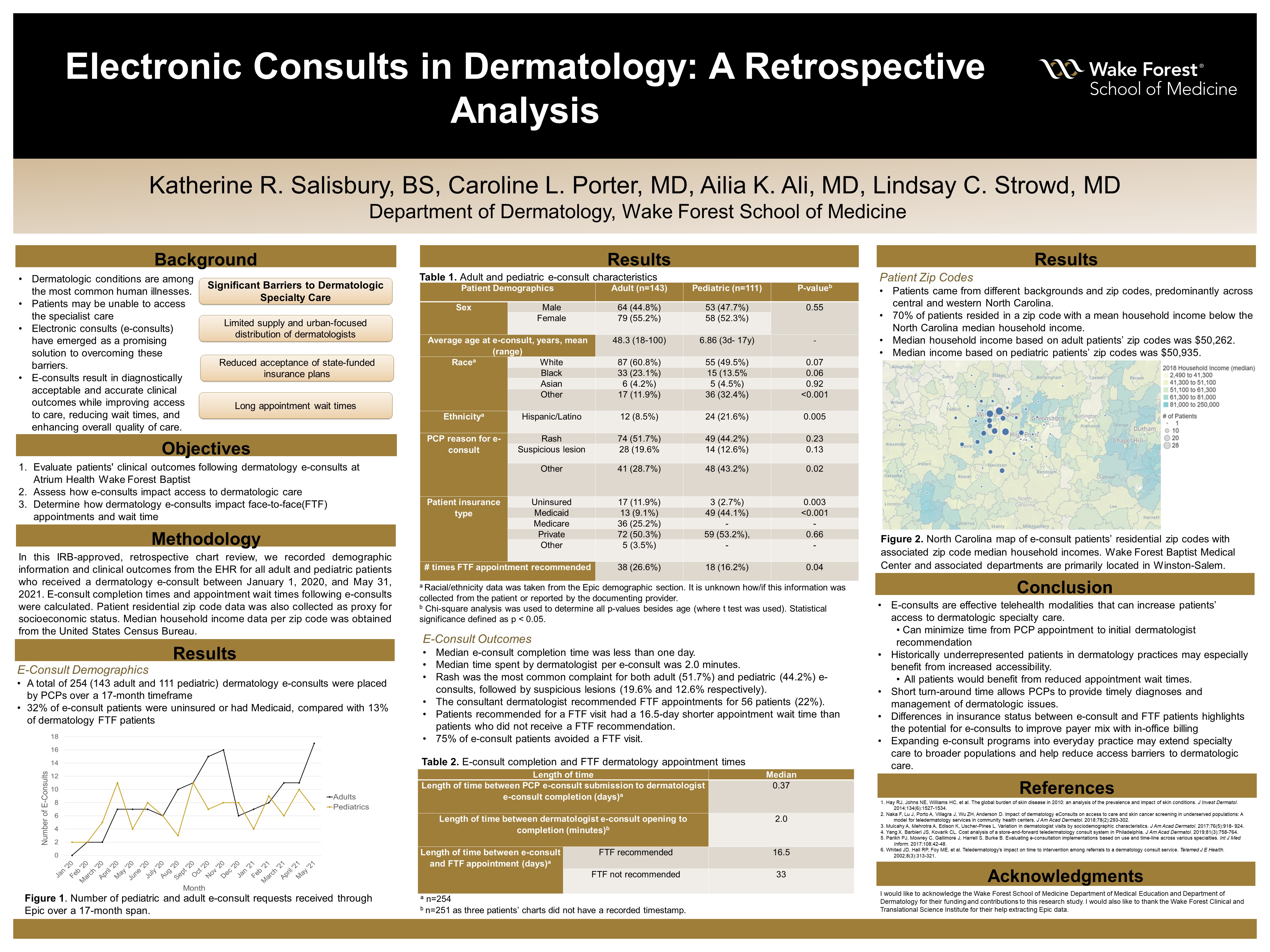
Background: Dermatologic conditions are among the most common human illnesses, affecting approximately one-third of individuals in the United States. Although nearly one in four office visits to physicians in the United States are for skin conditions, less than a third of those visits are with dermatologists. While many of these patients would prefer to see a dermatologist for their concerns, they may be unable to access specialist care. The limited supply and urban-focused distribution of dermatologists, reduced acceptance of state-funded insurance plans, and long appointment wait times all pose significant challenges to individuals seeking dermatologic care. Electronic consults (e-consults) have emerged as a promising solution to overcoming these barriers while providing high-quality dermatologic care to a large, diverse patient population. Primary care providers (PCPs) place the e-consult via the electronic health record (EHR) to dermatologists, who respond by answering questions, requesting more information or lesion documentation, and/or scheduling in-person visitations. These consults result in diagnostically acceptable and accurate clinical outcomes while improving access to care, reducing wait times, and enhancing overall quality of care.
Hypothesis: E-consults can be quickly completed by dermatologists and will reduce the required number of face-to-face (FTF) dermatology appointments as well as the appointment wait time for patients for whom a FTF appointment is recommended.
Methods: In this IRB-approved retrospective chart review, we recorded demographic information and clinical outcomes from the EHR for all adult and pediatric patients who received a dermatology e-consult between January 1, 2020, and May 31, 2021. E-consult completion times and appointment wait times following e-consults were calculated. Patient residential zip code data was collected for socioeconomic analysis. Median household income data per zip code was obtained from the United States Census Bureau.
Results: A total of 254 (143 adult and 111 pediatric) dermatology e-consults were placed by PCPs over the 17-month timeframe. Seventy percent of patients resided in a zip code with a mean household income below the North Carolina median household income. Thirty-two percent of e-consult patients were uninsured or had Medicaid, compared with 13% of dermatology FTF patients. The median e-consult completion time was less than one day. Rash was the most common complaint for both adult (51.7%) and pediatric (44.2%) e-consults. The consultant dermatologist recommended FTF appointments for 56 patients (22%). Patients recommended for a FTF visit had a 16.5-day shorter appointment wait time than patients who did not receive a FTF recommendation. Seventy-five percent of e-consult patients avoided a FTF visit, defined as not being seen by dermatology within 90 days of e-consult.
Conclusions: E-consults are effective telehealth modalities that can increase patients’ access to dermatologic specialty care while minimizing time from PCP appointment to initial dermatologist recommendation. Patients who are typically underrepresented in dermatology practices may especially benefit from the increased accessibility, and all patients requiring FTF visits may benefit from the reduced appointment wait time. The short turn-around time for e-consults allows PCPs to provide timely diagnoses and management of dermatologic issues. The differences in insurance status between e-consult and FTF patients highlights the potential for e-consults to improve payer mix with in-office billing. Integrating and expanding e-consult programs into everyday practice may extend specialty care to broader populations and help reduce access barriers to dermatologic care.
Source of funding or other support that funded this research: Department of Medical Education and Department of Dermatology, Wake Forest School of Medicine
-
Supporting Documents
- Electronic Consults in Dermatology: A Retrospective Analysis
Powered by Acadiate
© 2011-2024, Acadiate Inc. or its affiliates · Privacy
 CLOSE SIDEBAR
CLOSE SIDEBAR