Your message has been sent.
 CLOSE SIDEBAR
CLOSE SIDEBAR
Trabeculectomy Revision via Needling Augmented with Sub-conjunctival Mitomycin
Alexandria Marshall
Poster Title: Trabeculectomy Revision via Needling Augmented with Sub-conjunctival Mitomycin
Student: Alexandria Marshall, Class of 2023
Faculty Mentor and Department: J. Brett Bond, Ophthalmology
Funding Source: none
ABSTRACT
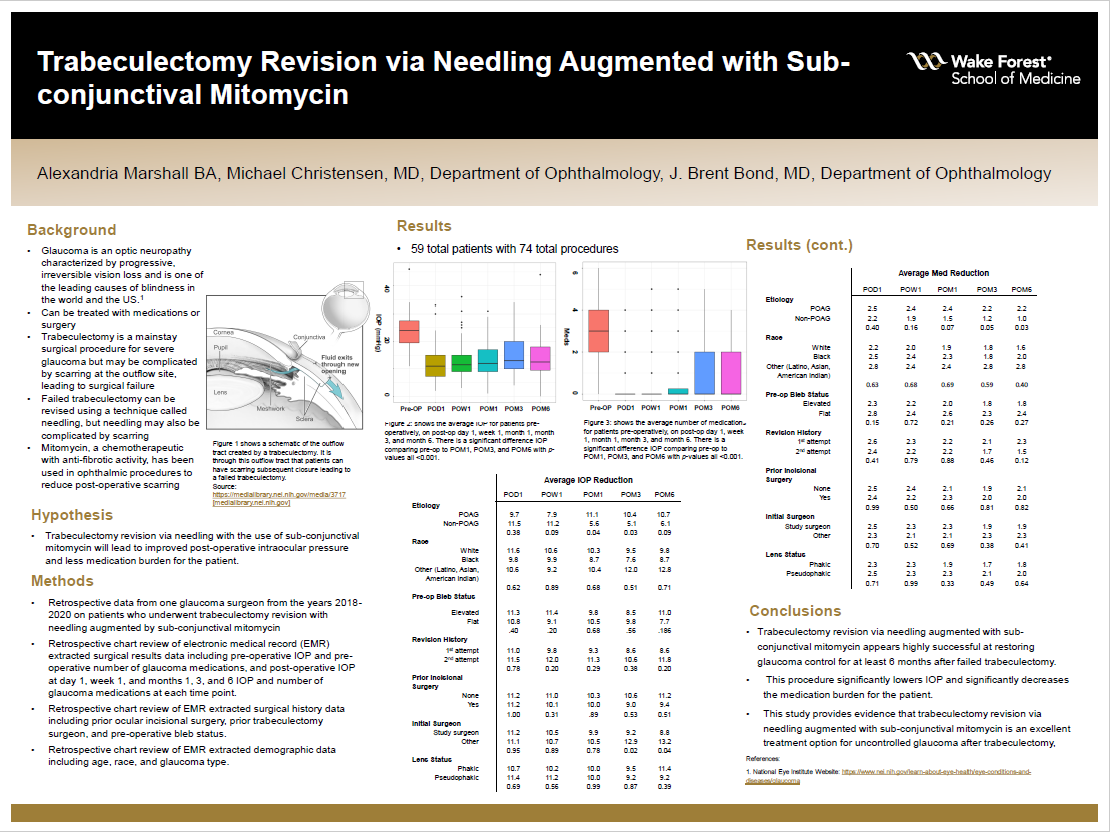
Background: Glaucoma, of which primary open-angle being the leading etiology, is one of the leading causes of blindness in the United States caused by an increase in intraocular pressure. Various medications and surgeries are the standards of care for treating glaucoma. Trabeculectomy is one of the main surgical techniques to treat severe glaucoma treated with maximum drops. While this surgical procedures boosts a high success rate, scarring of intraocular fluid flow tract is frequent complication, requiring further surgery. The subsequent surgery, sub-conjunctival needling, while also successful faces the same challenges as the initial trabeculectomy. Mitomycin, a chemotherapeutic, has been used in various ophthalmic procedures such as repeat LASIK to prevent scarring. This study looks at one surgeon’s success using sub-conjunctival mitomycin intra-operatively during needling.
Hypothesis: Trabeculectomy revision via needling with the use of sub-conjunctival mitomycin will lead to improved post-operative intraocular pressure readings and fewer glaucoma drops.
Methods: Patients who had previously undergone trabeculectomy revision with needling and sub-conjunctival needling during the years 2018-2020. Patients who had this procedure as well as a phaco-emulsification during the same operative visit were excluded. Each patient’s intraocular pressure (IOP) and glaucoma drop count were found for their pre-operative visit, post-operative day 1, week 1, month 1, month 3, and month 6. Data on whether this was a repeat needling procedure, the need for additional surgery within the 6 month time frame, prior incisional eye surgery, bleb status, lens status, and trabeculectomy surgeon was collected. If a patient required an additional surgery during the immediate 6 month post-operative period, their data was collected up to the point of their second surgery and then was excluded. Lastly demographic data such age, race, etiology, and year were taken.
Results: The records of 74 patients were taken across this 3-year period. The average pre-operative IOP (n=59) was 23.8 with 3 glaucoma drops. On post-operative day 1, the average IOP (n=58) was 11.8 with 0.5 glaucoma drops. On post-operative week 1 (n=58), month 1 (n=56), month 3 (n=53), and month 6 (n=48), the average IOPs were 13.0, 13.4, 15.0, and 13.7 respectively with the average number of glaucoma drops were 0.7, 0.7, 1.0, and 1.1 respectively. A Wilcoxon-ranked signed test showed the difference between pre-operative IOP and post-operative IOP at post-operative month 1, 3, and 6 to be significant (Z=-6.1, p <0.001; Z=-5.6, p <0.001; Z=-5.4, p <0.001). Additionally, the decrease in the number of post-operative glaucoma medications was also significant at post-operative month 1, 3, and 6 to be significant (Z=-5.7, p <0.001; Z=-5.1, p <0.001; Z=-5.2, p <0.001).
Conclusions: This study shows the success of trabeculectomy revision via needling using sub-conjunctival mitomycin across a 6 month period. Given the decrease in the average IOP and number of glaucoma drops shows that this procedure is largely effective in lowering intraocular and number of glaucoma drops. Additionally, these results were found regardless of a patient’s race, glaucoma etiology, age, revision history. This study offers an alternative management option for patients with worsening glaucoma with a failed trabeculectomy.
Source of mentor’s funding or other support that funded this research: None
-
Supporting Documents
- Trabeculectomy Revision via Needling Augmented with Sub-conjunctival Mitomycin
Powered by Acadiate
© 2011-2024, Acadiate Inc. or its affiliates · Privacy
