Your message has been sent.
 CLOSE SIDEBAR
CLOSE SIDEBAR
An Empirical Analysis on Medicare Payment Variations
Matthew Buddensick, Jake Varghese, Ai Ren (faculty mentor)
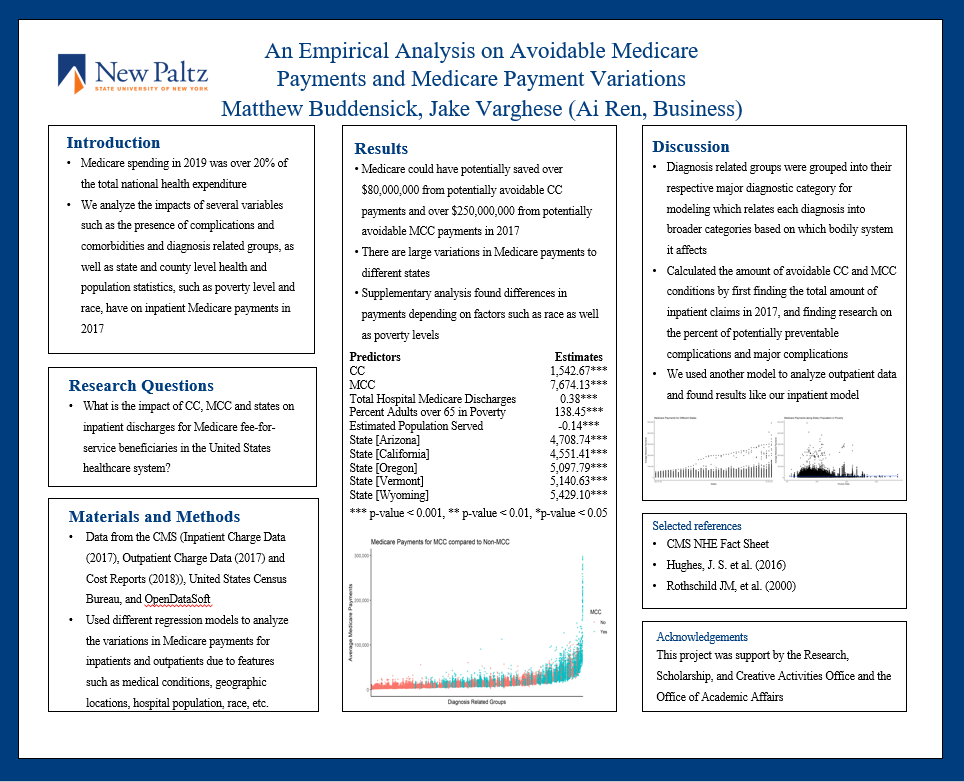
We studied the variations in Medicare payments and avoidable Medicare Payments. Specifically, we analyze the variations across Diagnosis Related Groupings (DRGs), Complications and Comorbidities (CC), Major Complications and Comorbidities (MCC), geographic areas, poverty, and race. We use Medicare Provider Utilization and Payment Inpatient and Outpatient Charge Data from The Centers for Medicare and Medicaid Services (CMS) in 2017, CMS Cost Reports Hospital Form 2552-10, County Population Totals: 2010-2019 reports from United States Census Bureau, and county level population health statistics. We introduce state-level fixed effects into our linear regression model and control for CC, MCC, race, poverty, income, and DRG categories. The impact of CC and MCC on Medicare payments are $1,542.67 (95% confidence interval [CI] $1,442.15 to $1,643.19, p-value < 0.001) and $7,674.13 (95% CI $7,578.02 to $7,770.24, p-value < 0.001) which quantifies the extra cost for CC and MCC conditions. The state-level fixed effects are statistically significant which implies Medicare payments do vary across states. The impact of Total Hospital Medicare Discharges is $0.38 (95% CI, $0.37 to $0.39, p-value < 0.001) which quantifies the negotiated power when hospitals go through the Medicare payment reimbursement process. Our results quantify the impact of CC and MCC on Medicare payments and suggest that, by reducing avoidable CC and MCC, Medicare can save over $330,000,000.
-
School Work
- An Empirical Analysis on Avoidable Medicare Payments and Medicare Payment Variations Poster
Media
- Elevator Talk for Matthew Buddensick and Jake Varghese
Powered by Acadiate
© 2011-2024, Acadiate Inc. or its affiliates · Privacy
