Your message has been sent.
 CLOSE SIDEBAR
CLOSE SIDEBAR
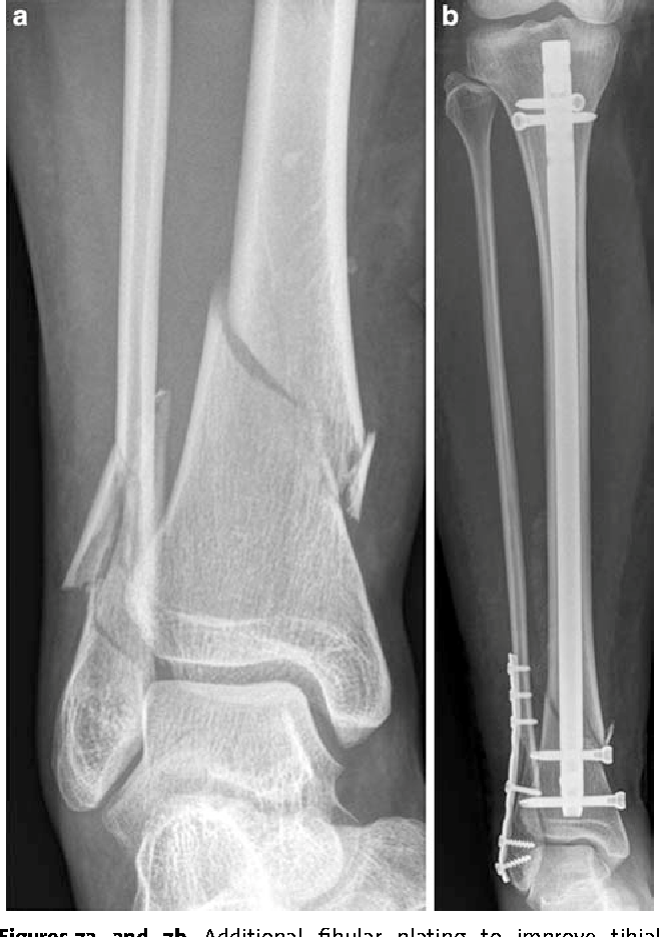
The Role of Fibula Fixation in Preventing Malalignment in Distal Third Tibia Fractures Treated with Intramedullary Nailing
Georges Abdelahad
ABSTRACT
Background: Distal third tibia and fibula fractures treated with intramedullary nailing can fail
into angular deformity despite appropriate nailing technique. The purpose of this study was to
examine variables specific to the injury pattern, nail placement, and whether fibula fixation
assisted in preventing post-operative angular deformity or catastrophic failure.
Hypothesis: Fibula fixation in distal third tibia fractures treated will intramedullary nailing will assist in preventing post-operative angular deformity or catastrophic failure.
Methods: We performed a retrospective chart review of all distal third tibia and fibula fractures
treated with intramedullary tibia nailing at a level 1 trauma center. Immediately post-operative
and 3-month imaging were examined to determine the distal nail location as well as any angular
deformity. Other demographic information, injury pattern, hardware failure, and infection
complications were documented. Regression analysis was performed to identify factors
associated with malalignment.
Results: 27 distal tibia-fibula fractures were identified, 3 of which had concurrent fibula fixation.
Fractures with a more unstable fracture pattern were statistically associated with malalignment.
Tibia nail endpoint was not associated with malalignment overall, however, among segmental
and highly comminuted fractures, tibia nail endpoint was statistically associated with
malalignment postoperatively. The addition of fibula fixation did not prevent malalignment. In
contrast, tibia nail endpoint did not affect malalignment in simple fractures.
Conclusions: This study highlights the importance of precise tibia nail endpoint particularly in the
setting of highly comminuted, unstable distal third tibia-fibula fractures. Furthermore, it suggests
that fixation of fibula fracture may not compensate for medial endpoint of tibia nail in preventing
malalignment. Catastrophic hardware failure was observed in a highly comminuted distal third
tibia fractures with associated simple fibula fracture that was not fixed, despite adequate tibia
nail endpoint. Although further research is warranted, these findings suggest that distal third
tibia-fibula fractures with more complex fracture characteristics may likely benefit from stiffer
constructs to prevent future deformity and catastrophic hardware failure.
Powered by Acadiate
© 2011-2024, Acadiate Inc. or its affiliates · Privacy
