Your message has been sent.
 CLOSE SIDEBAR
CLOSE SIDEBAR
A retrospective assessment of HIV screening efforts at Wake Forest Baptist Health
Allison Boone
Background: Southern states currently bear the greatest HIV burden in the United States. In 2016, 47% of deaths due to HIV occurred in the South, and over half of new diagnoses in 2017 were made in Southern states. Several factors distinguishing the South from other regions of the US may play a role in this regional disparity, including the relatively high proportion of people living in rural areas. This poses a unique challenge, as these individuals tend to have decreased access to healthcare providers locally and are less likely to have access to reliable transportation. Racial disparities in the South also play a significant role in access to HIV screening and care; African American men who have sex with men are particularly affected. Given the higher rates of HIV diagnosis and mortality in the South, screening efforts within hospital systems may be falling short of CDC guidelines for HIV screening. The objective of this study is to assess Wake Forest Baptist Health’s adherence to HIV screening recommendations outlined by the CDC and investigate if race, sex, and geographic location influence a person’s probability of being screened.
Hypothesis: We hypothesize that Wake Forest Baptist Health will fall short of the CDC’s guidelines and that the demographic factors mentioned previously will be strong predictive factors of this deficit.
Methods: Patient data, including address, sex, race, ethnicity, and birth date, for those who had an encounter in the WFBH system from January 1, 2018 – December 31, 2018 were obtained from Epic/Wake One and stored in REDCap. Patient addresses were identified as “rural” or “urban” using 2010 US Census data. Only patients ages 13 – 64 years of age at the time of their visit were included. Data were analyzed using Pearson’s Chi-squared test with significance defined as p<0.01 to account for multiple comparisons. Python, GraphPad and Excel were used in data processing and analysis.
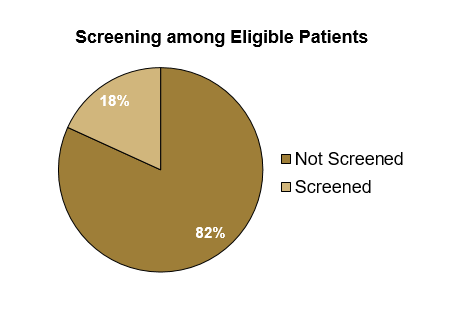
Results: Of the 138666 patients who met the CDC’s screening criteria, 18% were screened for HIV at WFBH. Patients living in urban areas were more likely than those in rural areas to be screened, at a rate of 24.7% and 14.0% respectively (p<0.0001). Females were also screened more frequently than men (20.8% vs. 13.9%; p<0.0001). Screening was not evenly distributed among races (p<0.0001), with African Americans screened at the highest rate, 33.9%. When broken down by type of residence, the rate of screening in African Americans residing in urban areas was lower than that of rural areas (29.1% vs 41.9%; p<0.0001). In other racial groups, those residing in urban areas were more likely or equally as likely to be screened compared to their rural counterparts. When considering ethnicity, Hispanic patients were screened at a higher rate than non-Hispanic patients (28.7% vs. 17.8%; p<0.0001).
Conclusions: These data indicate low rates of HIV screening among eligible patients receiving care at WFBH. Additionally, HIV screening at WFBH fits published trends indicating lower screening rates in rural areas versus urban areas. This trend held when accounting for sex and ethnicity, but was not consistent when considering race. Overall, these data indicate room for improvement in HIV screening efforts at WFBH.
Powered by Acadiate
© 2011-2024, Acadiate Inc. or its affiliates · Privacy
