Your message has been sent.
 CLOSE SIDEBAR
CLOSE SIDEBAR
Dance for Diabetes: A Study Design and Implementation Project Using Dance to Improve Diabetes Self-Management
Kychelle Del Rosario
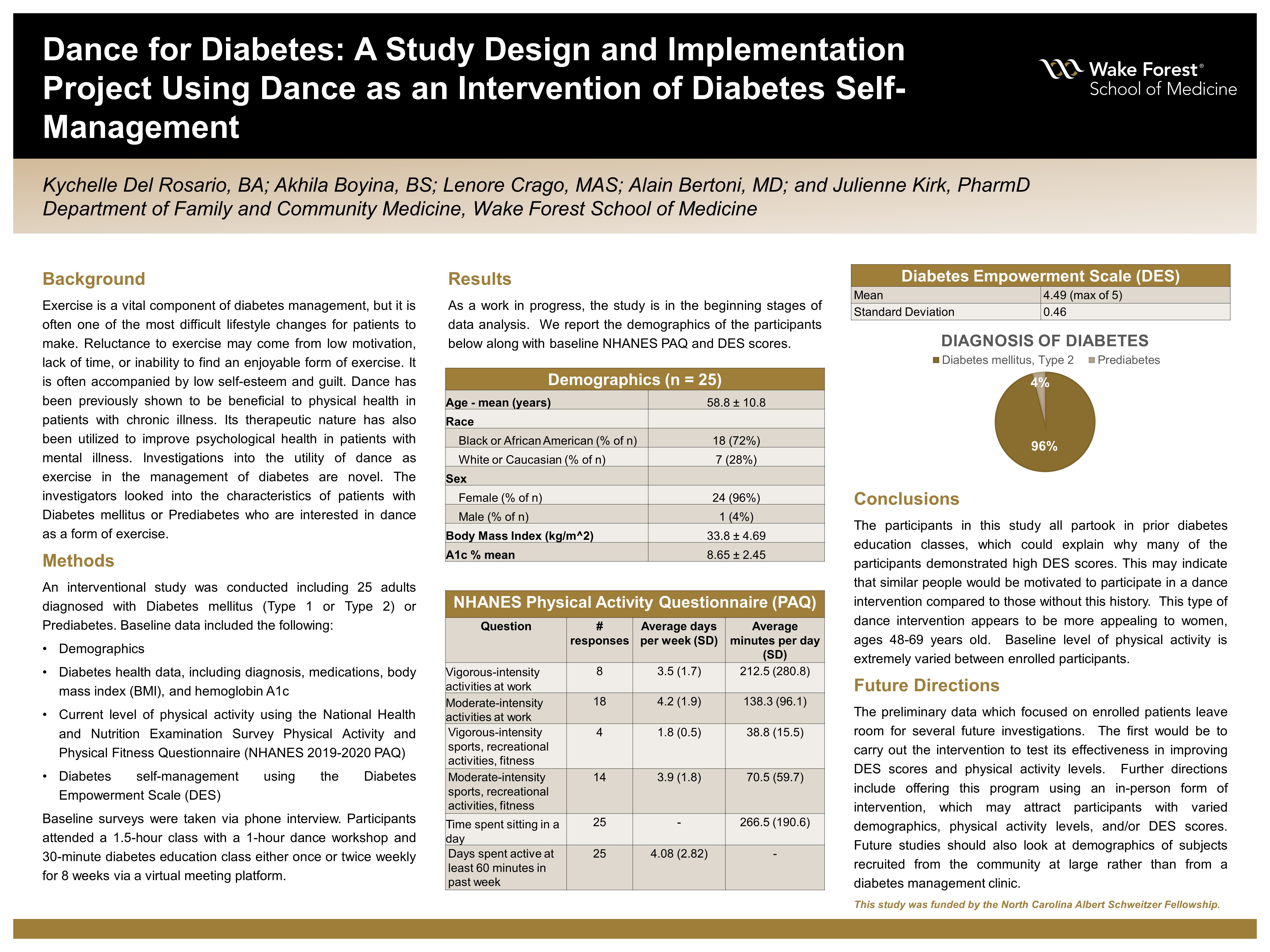
Background: Exercise is a vital component of diabetes management, but it is often one of the most difficult lifestyle changes for patients to make. Reluctance to exercise may come from low motivation, lack of time, or inability to find an enjoyable form of exercise. It is often accompanied by low self-esteem and guilt. Dance has been previously shown to be beneficial to physical health in patients with chronic illness. Its therapeutic nature has also been utilized to improve psychological health in patients with mental illness. Investigations into the utility of dance as exercise in the management of diabetes are novel. The investigators looked into the characteristics of patients with diabetes mellitus or prediabetes who are interested in dance as a form of exercise.
Hypothesis: Patients with diabetes who are highly empowered to take care of their diabetes are more likely to enroll in a dance intervention for diabetes management.
Methods: An interventional study was conducted including 25 adults diagnosed with diabetes mellitus (Type 1 or Type 2) or prediabetes. Baseline data on demographics and diabetes health [including diagnosis, medications, body mass index (BMI), hemoglobin A1c] were obtained from chart review. Initial surveys regarding current level of physical activity using the National Health and Nutrition Examination Survey Physical Activity and Physical Fitness Questionnaire (NHANES 2019-2020 PAQ) and self-perception of the quality of diabetes self-management using the Diabetes Empowerment Scale (DES) were taken via phone interview. Participants attended a 1.5-hour class with a 1-hour dance workshop and 30-minute diabetes education class either once or twice weekly for 8 weeks via a virtual meeting platform.
Results: The 25 participants that were a part of the study were very similar in terms of demographic data. The mean age was 58.8 years with a standard deviation of 10 years. All but one of the participants were female. All of the participants were diagnosed with Type 2 diabetes except for one with prediabetes. The BMI of participants was variable at 33.8 with a standard deviation of 4.69. All of the participants that attended 1 or more classes of the intervention were patients who had attended or were currently attending diabetes education classes. The mean Diabetes Empowerment Scale (DES) score was 4.51 out of max score of 5, with a standard deviation of 0.45.
Conclusions: The high DES scores and history of diabetes education in the participants of the study indicate that similar people would be motivated to participate in a dance intervention compared to those without this history. This type of dance intervention appears to be more appealing to women, ages 40-60 years old.
Source of mentor’s funding or other support that funded this research: North Carolina Albert Schweitzer Fellowship.
Powered by Acadiate
© 2011-2024, Acadiate Inc. or its affiliates · Privacy
